Physiotherapy And Nutrition Course Details
Physiotherapy and Nutrition Course. Mobile Phone 019699947171, 01797522136, 01987073965. The most vital Diploma Course in Medical Science is the Diploma in Physiotherapy and Nutrition Course. Maximum problems and diseases may be eradicated through physiotherapy and nutrition. So, the Study of Physiotherapy and Nutrition Courses is essential.

Physiotherapy and Nutrition Course 1 Year, Physiotherapy and Nutrition Course 2 Years, Physiotherapy and Nutrition Course 3 Years, and Physiotherapy and Nutrition Course 4 Years. All these courses are available at HRTD Medical Institute. HRTD Medical Institute is an Organization of HRTD Limited.
Physiotherapy and Nutrition Course 1 Year (Short Diploma)
This Course Contains 10 Subjects. Total Course Fee Tk 52500/- including admission fee tk 10500/-, monthly fee tk 3000, and exam fee. Total exam marks 1000, and pass marks 33 per subject. The subjects are Human Anatomy and Physiology, Pharmacology, First Aid, Study of Disease, Massage Therapy, Exercise Therapy, Electrotherapy, Food and Nutrition, Vitamin Deficiency Diseases, and Hyper Vitaminosis.
Physiotherapy and Nutrition Course 2 Years (Short Diploma)
This Course Contains 18 Subjects. Total Course Fee Tk 92500/- including admission fee tk 16500/-, monthly fee tk 3000, and exam fee. Total exam marks 1800, and pass marks 33 per subject. The subjects are Human Anatomy and Physiology, Pharmacology, First Aid, Study of Disease, Massage Therapy, Exercise Therapy, Electrotherapy, Food and Nutrition, Vitamin Deficiency Diseases, Hyper Vitaminosis, Carbohydrate Metabolic Disease, Protein Metabolic Disease, Fat Metabolic Disease. Physiotherapy for Pain Management, etc.
Physiotherapy and Nutrition Course 3 Years (Long Diploma)
This Course Contains 24 Subjects. Total Course Fee Tk 142500/- including admission fee tk 20500/-, monthly fee tk 3000, and exam fee. Total exam marks 2400, and pass marks 33 per subject. The subjects are Human Anatomy and Physiology, Pharmacology, First Aid, Study of Disease, Massage Therapy, Exercise Therapy, Electrotherapy, Food and Nutrition, Vitamin Deficiency Diseases, Hyper Vitaminosis, Carbohydrate Metabolic Disease, Protein Metabolic Disease, and Fat Metabolic Disease. Physiotherapy for Pain Management, etc.
Physiotherapy and Nutrition Course 4 Years (Diploma)
This Course Contains 30 Subjects. Total Course Fee Tk 182500/- including admission fee tk 30500/-, monthly fee tk 3000, and exam fee. Total exam marks 3000, and pass marks 33 per subject. The subjects are Human Anatomy and Physiology, Pharmacology, First Aid, Study of Disease, Massage Therapy, Exercise Therapy, Electrotherapy, Food and Nutrition, Vitamin Deficiency Diseases, Hyper Vitaminosis, Carbohydrate Metabolic Disease, Protein Metabolic Disease, Fat Metabolic Disease. Physiotherapy for Pain Management, etc.
Total Subjects for Physiotherapy and Nutrition Courses
- Human Anatomy and Physiology,
- Pharmacology,
- First Aid, Study of Disease,
- Massage Therapy,
- Exercise Therapy-1
- Electrotherapy,
- Gastrology
- Food and Nutrition,
- Cardiology
- Vitamin Deficiency Diseases,
- Mineral Deficiency Diseases,
- Medical Diagnosis-1
- Exercise Therapy-2
- Orthopedics
- Hyper Vitaminosis & Treatment
- Carbohydrate Metabolic Disease,
- Protein Metabolic Disease,
- Fat Metabolic Disease.
- Electrotherapy-2
- Medical Diagnosis-2
- Neurology
- Physiotherapy for Pain Management,
- Endocrinology
- Physiotherapy for Paralysis Management, etc.
Location for the Best Physiotherapy and Nutrition Course
HRTD Medical Institute, Abdul Ali Madbor Mansion, Section-6, Block-Kha, Road-1, Plot-11, Metro Rail Piller No. 249, Mirpur-10 Golchattar, Dhaka-1216. It is just South Side of Fire Serve, Islami Bank, Janata Bank and Medinova, North Side of Sundorbon Qureer Service and Folpotty Mosjit Gorosthan, West Side of Agrani Bank, Teletalk Customer Care, East Side of Maliha Apartment.

Physiotherapy and Nutrition Chamber Starting & Establishment
After completing the Physiotherapy and Nutrition Course ( 3 Years Or, 4 Years Diploma ) you can start a Physiotherapy and Nutrition Chamber in any location of Bangladesh. You need to obtain The Registration and The License from the Respective Authority of the Government of the People's Republic of Bangladesh. We only help our students obtain registration and licenses for the Starting & Establishment of Physiotherapy and Nutrition Chamber.
ফিজিওথেরাপি ও নিউট্রিশন কোর্স (৩ বছর বা ৪ বছরের ডিপ্লোমা) শেষ করার পর আপনি বাংলাদেশের যেকোনো স্থানে একটি ফিজিওথেরাপি এবং নিউট্রিশন চেম্বার শুরু করতে পারেন। আপনাকে গণপ্রজাতন্ত্রী বাংলাদেশ সরকারের সংশ্লিষ্ট কর্তৃপক্ষের কাছ থেকে নিবন্ধন এবং লাইসেন্স পেতে হবে। আমরা শুধুমাত্র আমাদের ছাত্রদের ফিজিওথেরাপি ও নিউট্রিশন চেম্বারের শুরু ও প্রতিষ্ঠার জন্য নিবন্ধন এবং লাইসেন্স পেতে সাহায্য করি।
Why Physiotherapy and Nutrition Diploma in the Best Diploma Course
This course contains some subjects in physiotherapy and some subjects in nutrition. Physiotherapy is an excellent treatment for pain management. Physiotherapy is classified into 3 types. Massage Therapy, Exercise Therapy, and Electro Therapy. Physiotherapy reduces the use of Medicine that destroys the vital organs of the human body. Nutritional subjects are important for the prevention of many diseases. Nutrition will help to treat many deficiency diseases. and diseases due to the high intake of food.
What is a Balanced Diet?
The diet that is actually required for a body is called a balanced diet. Both access and deficiency of anything are bad. This is true for our body while eating or drinking. So, understanding actual calculations while dieting is important.
Teacher for Physiotherapy and Nutrition Course
Dr. Md. Sakulur Rahman, MBBS, CCD (BIRDEM)
Dr. Disha, MBBS, FCPS ( FP)
Dr. Tisha, MBBS, PGT Medicine
Dr. Anika, MBBS, PGT Medicine
Dr. Sanjana, BDS, PGT, MPH
Dr. Juthi, BDS, PGT
Dr. Keya, BDS, PGT Dental Surgery
Dr. Mahinul Islam, MBBS, PGT
Dr. Rayhan, BPT ( Bachelor of Physiotherapy)
Dr. Abu Hurayra, BPT ( Bachelor of Physiotherapy)
Dr. Suhana, MBBS, PGT Gyne and Medicine
Dr. Lamia, MBBS
Dr. Shamima, MBBS, PGT Gyne and Medicine
Dr. Sharmin Ankhi, MBBS, PGT Medicine
Dr. Danial Hoque, MBBS, C-Card ( Heart Foundation)
Dr. Farhana, MBBS, PGT
Dr. Benzir, MBBS, FCPS ( FP)
Dr. Amena Afroze Anu, MBBS, PGT Gyne and Medicine
Dr. Turzo, MBBS, PGT Medicine
Other Medical Courses of HRTD Medical Institute
Paramedical Course, Diploma Medical Assistant Course, Diploma in Medicine and Surgery, Diploma in Paramedical, DMDS Course, Nursing Course, Pathology Course, Physiotherapy Course, Post Diploma Training Course, PDT Cardiology, PDT Diabetology, PDT Orthopedics, PDT Medicine, PDT Dermatology, PDT Gastrology, PDT Neurology, PDT Pediatrics, PDT Ophthalmology, PDT Eear Nose and Throat, PDT Skin VD, PDT Physiotherapy, PDT Gynecology, PDT Maternal & Child Health, Pharmacy Course, Caregiver Course, RMP Course, LMAF Course, etc.
Human Anatomy and Physiology for Physiotherapy and Nutrition Course
The study of Body Structure and its functions is Anatomy and Physiology. Here we discuss the systems of the Human Body and its Organs, Tissues, and Cells. The systems of the Human Body are the Digestive System, Respiratory System, Cardiovascular System, Skeletal System, Muscular System, Nervous System, Endocrine System, Immune System, Lymphatic System, Integumentary System, and Urinary System.
Pharmacology-1 for Physiotherapy and Nutrition Course
Physiotherapy and Nutrition Course. The study of Drugs and Medicine is called Pharmacology. Here we discuss group-wise drugs and their medicines in Pharmacology-1. Common Groups of Drugs are Pain Killer Drugs, Anti Ulcer Drugs, Anti Vomiting Drugs, Laxative Drugs, Motility Drugs, Antimotility Drugs, Bronchodilator Drugs, Antibiotic Drugs, Anti Fungal Drugs, Anti Protozoal Drugs, Anti Viral Drugs, Anthelmintic Drugs, Anti Hypertensive Drugs, Beta Blocker Drugs, Calcium Channel Blocker Drugs, ACE Inhibitor Drugs, Hemostatic Drugs, Analgesic Drugs, Antipyretic Drugs, Anti Thrombotic Drugs, etc.
First Aid for Physiotherapy and Nutrition Course
Physiotherapy and Nutrition Course. First Aid is an important subject for Medical Courses including Diplomas in Medicine& Surgery Course, RMP Courses, LMAF Courses, Paramedical Courses, DMA Courses, DMS Courses, Nursing Courses, Dental Courses, Pathology Courses, Physiotherapy Courses, Caregiver Courses, etc. Here we discuss Shock, Classification Shock, Causes of Shock, Stages of Shock, Clinical Features of Shock, Hypovolemic Shock, Cardiogenic Shock, Neurogenic Shock, Traumatic Shock, Burn Shock, Electric Shock, Psychogenic Shock, Anaphylactic Shock, First Aid of Shock, First Aid of Cut, First of Snake Bite, First Aid of Accidental Injury, etc.
Study of OTC Drugs for Physiotherapy and Nutrition Course
Physiotherapy and Nutrition Course. OTC Drugs are important for all Medical Assistant Courses, Diploma Medical Courses, LMAF Courses, and RMP Courses. It is also important for the Physiotherapy and Nutrition Course. These OTC Drugs can be sold or purchased without any prescription from Registered MBBS Doctors. These Drugs are Emergency and Safe for the patients. The study of OTC Drugs improves the quality of practice. Some OTC Drugs are Albendazole, Ascorbic Acid, Calcium, Multivitamins, Vitamin B Complex, Omeprazole, Oral Rehydration Salt, Salbutamol, etc.
OTC ড্রাগগুলি সমস্ত মেডিকেল অ্যাসিস্ট্যান্ট কোর্স, ডিপ্লোমা মেডিকেল কোর্স, LMAF কোর্স এবং RMP কোর্সের জন্য গুরুত্বপূর্ণ। এটি ফিজিওথেরাপি এবং পুষ্টি কোর্সের জন্যও গুরুত্বপূর্ণ। এই OTC ওষুধগুলি নিবন্ধিত এমবিবিএস ডাক্তারদের কাছ থেকে কোনও প্রেসক্রিপশন ছাড়াই বিক্রি বা কেনা যায়। এই ওষুধগুলি জরুরী এবং রোগীদের জন্য নিরাপদ। ওটিসি ওষুধের অধ্যয়ন অনুশীলনের মান উন্নত করে। কিছু ওটিসি ওষুধ হল অ্যালবেনডাজল, অ্যাসকরবিক অ্যাসিড, ক্যালসিয়াম, মাল্টিভিটামিন, ভিটামিন বি কমপ্লেক্স, ওমেপ্রাজল, ওরাল রিহাইড্রেশন সল্ট, সালবুটামল ইত্যাদি।
Hematology and Pathology for Physiotherapy and Nutrition Course
Physiotherapy and Nutrition Course. The study of Blood and Blood Disease is called Hematology and the Study of Pathos and Process of Disease Creation and Diagnosis is called Pathology. In Hematology and Pathology, we discuss blood cells, their structure and functions, Blood Diseases, Common Pathos and their pathogenesis, Atrophy, Hypertrophy, Metaplasia, Gangrene, Pathological Tests like TC, DC, ESR, Hemoglobin Percentage, etc.
রক্ত ও রক্তের রোগের অধ্যয়নকে বলা হয় হেমাটোলজি এবং স্টাডি অফ প্যাথোস এবং রোগ সৃষ্টি ও নির্ণয়ের প্রক্রিয়াকে প্যাথলজি বলা হয়। হেমাটোলজি এবং প্যাথলজিতে, আমরা রক্তের কোষ, তাদের গঠন এবং কার্যকারিতা, রক্তের রোগ, সাধারণ প্যাথোস এবং তাদের প্যাথোজেনেসিস, অ্যাট্রোফি, হাইপারট্রফি, মেটাপ্লাসিয়া, গ্যাংগ্রিন, প্যাথলজিকাল টেস্ট যেমন TC, DC, ESR, হিমোগ্লোবিন শতাংশ ইত্যাদি নিয়ে আলোচনা করি।
Microbiology, Antimicrobial Drugs and Nutrition Deficiency for Physiotherapy and Nutrition Course
Physiotherapy and Nutrition Course. The Study of Microorganisms is called Microbiology. The Drugs that are used for the treatment of Infectious Diseases are Antimicrobial Drugs. Microorganisms are Bacteria, Protozoa, Fungus, and Virus. Antimicrobial Drugs are Antibiotic Drugs ( Antibacterial Drugs), Anti Protozoal Drugs, Anti Fungal Drugs, and Anti Viral Drugs.
অণুজীবের অধ্যয়নকে মাইক্রোবায়োলজি বলা হয়। সংক্রামক রোগের চিকিত্সার জন্য যে ওষুধগুলি ব্যবহার করা হয় তা হল অ্যান্টিমাইক্রোবিয়াল ড্রাগ। অণুজীব হল ব্যাকটেরিয়া, প্রোটোজোয়া, ফাঙ্গাস এবং ভাইরাস। অ্যান্টিমাইক্রোবিয়াল ড্রাগগুলি হল অ্যান্টিবায়োটিক ড্রাগস (অ্যান্টিব্যাকটেরিয়াল ড্রাগস), অ্যান্টি প্রোটোজোয়াল ড্রাগস, অ্যান্টি ফাঙ্গাল ড্রাগস এবং অ্যান্টি ভাইরাল ড্রাগস।
Antibacterial Drugs are Azithromycin, Erythromycin, Clarithromycin, Cefaclor, Cefixime, Cefuroxime, Ceftriaxone, Ciprofloxacin, Moxifloxacin, Doxicicline, Gentamycin, Neomycin, Flucloxacillin, Amoxicillin, Clindamycin, etc.
ব্যাকটেরিয়ারোধী ওষুধগুলি হল Azithromycin, Erythromycin, Clarithromycin, Cefaclor, Cefixime, Cefuroxime, Ceftriaxone, Ciprofloxacin, Moxifloxacin, Doxicicline, Gentamycin, Neomycin, Flucloxacillin, Amoxicillin, Clindamycin, ইত্যাদি।
Anti protozoal Drugs are Metronidazole, Secnidazole, Tinidazole, Ornidazole, Nitazoxanide, etc. Antifungal Drugs are Fluconazole, Ketoconazole, Itraconazole, Econazole, Miconazole, Terbinafine, etc.
অ্যান্টি প্রোটোজল ড্রাগগুলি হল মেট্রোনিডাজল, সেকনিডাজল, টিনিডাজল, অর্নিডাজল, নাইটাজক্সানাইড ইত্যাদি। অ্যান্টিফাঙ্গাল ড্রাগগুলি হল ফ্লুকোনাজোল, কেটোকোনাজোল, ইট্রাকোনাজোল, ইকোনাজোল, মাইকোনাজোল, টেরবিনাফাইন ইত্যাদি।
When suffering from infections with microorganisms and during treatment with antimicrobial drugs, patients lose vitamins, minerals, and other nutrients. So, the Study of Microbiology, Antimicrobial Drugs, and Nutrition Supplement are essential for the proper treatment of patient infectious diseases.
অণুজীবের সংক্রমণে এবং অ্যান্টিমাইক্রোবিয়াল ওষুধের সাথে চিকিত্সার সময় রোগীরা ভিটামিন, খনিজ এবং অন্যান্য পুষ্টি হারান। সুতরাং, রোগীর সংক্রামক রোগের সঠিক চিকিৎসার জন্য মাইক্রোবায়োলজি, অ্যান্টিমাইক্রোবিয়াল ড্রাগস এবং নিউট্রিশন সাপ্লিমেন্টের অধ্যয়ন অপরিহার্য।
Practice of Medicine for Physiotherapy and Nutrition Course
Physiotherapy and Nutrition Course. The study of Disease and Treatment is called the Practice of Medicine. This subject is important for all medical practitioners, Diploma Medical Practitioners, Diploma Medical Assistants, and Rural Medical Practitioners. This subject is also important for all medical-related workers, nurses, and pharmacists to understand the movement of disease and treatment.
রোগ এবং চিকিত্সার অধ্যয়নকে মেডিসিনের অনুশীলন বলা হয়। এই বিষয়টি সকল মেডিকেল প্র্যাকটিশনার, ডিপ্লোমা মেডিকেল প্র্যাকটিশনার, ডিপ্লোমা মেডিকেল অ্যাসিস্ট্যান্ট এবং গ্রামীণ চিকিৎসা অনুশীলনকারীদের জন্য গুরুত্বপূর্ণ। রোগ এবং চিকিত্সার গতিবিধি বোঝার জন্য সমস্ত চিকিৎসা-সম্পর্কিত কর্মী, নার্স এবং ফার্মাসিস্টদের জন্যও এই বিষয়টি গুরুত্বপূর্ণ।
This subject discusses some common diseases. The discussion points for the Practice of Medicine are the Definition of Disease, Causes of Disease, Clinical Features of Disease ( Symptoms and Signs), Investigation of Disease, Treatment of Disease, Complication of Disease, and Advice for the Patients.
এই বিষয়ে কিছু সাধারণ রোগ নিয়ে আলোচনা করা হয়েছে। মেডিসিন অনুশীলনের আলোচনার বিষয়গুলি হল রোগের সংজ্ঞা, রোগের কারণ, রোগের ক্লিনিক্যাল বৈশিষ্ট্য (লক্ষণ এবং চিহ্ন), রোগের তদন্ত, রোগের চিকিৎসা, রোগের জটিলতা এবং রোগীদের জন্য পরামর্শ।
Medical Diagnosis for Physiotherapy and Nutrition Course
Physiotherapy and Nutrition Course. Medical diagnosis is a foundational subject in medicine focused on identifying the cause of a patient’s illness through systematic analysis of symptoms, signs, and tests. It spans basic science, laboratory technology, and clinical reasoning.
Here are the main topics and key areas of study in medical diagnostics:
1. Core Diagnostic Methodologies (The Diagnostic Process)
- Patient History and Clinical Interview: Eliciting subjective data, understanding patient complaints.
- Physical Examination: Gathering objective data via inspection, palpation, percussion, and auscultation.
- Differential Diagnosis: Comparing and contrasting multiple possible explanations for signs and symptoms to reach a, or rank, potential diagnoses.
- Diagnostic Reasoning/Pattern Recognition: Using experience to recognize common patterns of disease, rather than just analytical, step-by-step logic.
- Clinical Decision Support Systems: Using AI and algorithmic models to support diagnosis.
2. Clinical Laboratory Sciences (Laboratory Medicine)
- Hematology: Anemia, leukemia, lymphoma, multiple myeloma, bleeding, and coagulation disorders.
- Clinical Chemistry: Analysis of blood, urine, feces, and other body fluids for metabolic, liver, and kidney function (e.g., electrolytes, glucose, enzymes).
- Microbiology and Infectious Diseases: Identification of bacterial, viral, fungal, and parasitic infections (e.g., malaria, tuberculosis, HIV, COVID-19).
- Immunology and Serology: Testing for autoimmune diseases, antibody levels, and immune responses.
- Immunohematology (Blood Bank): Blood grouping, antibody screening, and transfusion compatibility.
- Cytology and Histopathology: Analysis of tissue samples and cells to diagnose cancer and tissue damage.
3. Medical Imaging and Radiology
- Radiography (X-ray): Standardized imaging for fractures, infections, or abnormalities.
- Computed Tomography (CT Scans): Detailed cross-sectional images for head, spinal, and abdominal assessment.
- Magnetic Resonance Imaging (MRI): Detailed imaging of soft tissues, brain, joints, and organs.
- Ultrasound (Sonography): Non-invasive imaging for cardiovascular, abdominal, and gynecological issues.
- Nuclear Medicine (PET Scans): Functional imaging to detect metabolic activity, seizures, and tumors.
4. Specialized Diagnostic Areas
- Molecular Diagnostics/Genetics: Chromosomal analysis, PCR (Polymerase Chain Reaction) for detecting genetic markers, and infectious diseases.
- Electrophysiology/Electrodiagnostics: Measuring electrical activity in the heart (ECG), brain (EEG), or nerves (nerve conduction studies).
- Endoscopy: Using specialized scopes to visualize internal organs, such as gastroscopy or colonoscopy.
- Cardiovascular Diagnostics: Cardiac catheterization, stress tests, and echocardiography.
5. Essential Principles and Quality Assurance
- Performance Metrics: Understanding sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV).
- Pre-analytical, Analytical, and Post-analytical Phases: Ensuring quality from sample collection through analysis to reporting.
- Medical Ethics and Patient Safety: Handling confidential information, avoiding misdiagnosis, and navigating informed consent.
- Overdiagnosis and Diagnostic Errors: Managing the risk of identifying diseases that will not cause symptoms in a patient’s lifetime, or missing a diagnosis.
6. Common Clinical Systems Studied
- Cardiovascular System: Acute Myocardial Infarction, Congestive Heart Failure.
- Respiratory System: Pneumonia, COPD, Asthma, Pulmonary Embolism.
- Renal System: Acute Kidney Injury, Nephrotic Syndrome, Chronic Renal Failure.
- Endocrinology: Diabetes mellitus, thyroid disorders, Addison’s disease.
- Gastroenterology: Liver abscess, Cirrhosis, Pancreatitis, inflammatory bowel disease.
These topics ensure that students understand both the “how” (techniques) and “why” (pathophysiology) of diagnostic medicine.
Dermatology for Physiotherapy and Nutrition Course
Physiotherapy and Nutrition Course. Dermatology. Mobile Phone Number 01797522136, 01987073965. The study of Skin Anatomy, Skin physiology, Skin Diseases, Diagnosis of Skin Diseases, Treatment of Skin Diseases, Complications of Skin Diseases, and Prevention of Skin Diseases is called Dermatology.
চর্মরোগবিদ্যা। মোবাইল ফোন নম্বর 01797522136, 01987073965। স্কিন অ্যানাটমি, স্কিন ফিজিওলজি, চর্মরোগ, চর্মরোগ নির্ণয়, চর্মরোগের চিকিৎসা, চর্মরোগের জটিলতা এবং চর্মরোগ প্রতিরোধের গবেষণাকে ডার্মাটোলজি বলা হয়।
Skin is the largest monitor of the human body for seeing and diagnosing body conditions and diseases. So, Every Medical practitioner, Medical Assistant, Nurse, Pharmacist, and highly skilled caregiver should study dermatology according to their related working field.
শরীরের অবস্থা এবং রোগগুলি দেখার এবং নির্ণয়ের জন্য ত্বক মানবদেহের সবচেয়ে বড় মনিটর। সুতরাং, প্রত্যেক চিকিৎসা চিকিৎসক, চিকিৎসা সহকারী, নার্স, ফার্মাসিস্ট এবং অত্যন্ত দক্ষ পরিচর্যাকারীর তাদের সংশ্লিষ্ট কর্মক্ষেত্র অনুযায়ী চর্মবিদ্যা অধ্যয়ন করা উচিত।
Common Skin diseases and disorders are Tineasis, Candidiasis, Acne, Cold Sore, Blister, Hives, Actinic keratosis, Rosacea, Carbuncle, Latex allergy, Eczema, Psoriasis, Cellulitis, Measles, Basal cell carcinoma, Squamous cell carcinoma, Melanoma, Lupus, Contact dermatitis, Vitiligo, Warts, Chickenpox, Seborrheic eczema, Keratosis pilaris, Ringworm, Melasma, Impetigo, Temporary skin disorders, and Permanent Skin disorders. For more information, there are some courses at HRTD Medical Institute. These Courses are PDT Dermatology, PDT Skin VD, and PDT Medicine.
সাধারণ চর্মরোগ এবং ব্যাধিগুলি হল টিনিয়াসিস, ক্যানডিডিয়াসিস, ব্রণ, কোল্ড সোর, ফোস্কা, আমবাত, অ্যাক্টিনিক কেরাটোসিস, রোসেসিয়া, কার্বাঙ্কল, ল্যাটেক্স অ্যালার্জি, একজিমা, সোরিয়াসিস, সেলুলাইটিস, হাম, বেসাল সেল কার্সিনোমা, স্কোয়ামাস সেল কার্সিনোমা, মেলানোমা, যোগাযোগ ডার্মাটাইটিস, ভিটিলিগো, ওয়ার্টস, চিকেনপক্স, সেবোরিক একজিমা, কেরাটোসিস পিলারিস, দাদ, মেলাসমা, ইমপেটিগো, অস্থায়ী ত্বকের ব্যাধি এবং স্থায়ী ত্বকের ব্যাধি। আরও তথ্যের জন্য, HRTD মেডিকেল ইনস্টিটিউটে কিছু কোর্স রয়েছে। এই কোর্সগুলি হল পিডিটি ডার্মাটোলজি, পিডিটি স্কিন ভিডি, এবং পিডিটি মেডিসিন।
Neurology for Physiotherapy and Nutrition Course
Neurology is a broad medical discipline focused on the diagnosis and management of disorders of the nervous system (brain, spinal cord, and peripheral nerves). Key topics include the neurological examination, cerebrovascular diseases (stroke), epilepsy, neurodegenerative disorders, and neuromuscular diseases.
Here are the main topics in neurology, categorized by subject area:
1. Fundamental Neurology and Clinical Skills
- Neurological Examination: Mental status examination (level of alertness, cognition), cranial nerve assessment (I-XII), motor system (strength, tone), reflexes, sensation, coordination, and gait analysis.
- Neuroanatomy & Localization: Understanding cortical, brainstem, spinal cord, and peripheral nervous system localization.
- Neuroimaging & Investigations: Interpreting CT scans, MRIs, angiography, lumbar puncture (CSF analysis), electroencephalography (EEG), and electromyography (EMG)/nerve conduction studies.
- Upper vs. Lower Motor Neuron Lesions: Differentiating findings (hyperreflexia/spasticity vs. atrophy/fasciculations).
2. Major Neurological Disorders (Disease Specific)
- Stroke and Cerebrovascular Disease: Ischemic stroke, hemorrhagic stroke, Transient Ischemic Attack (TIA), venous thrombosis, and NIH stroke scale management.
- Epilepsy and Seizure Disorders: Generalized vs. focal seizures, epilepsy syndromes, status epilepticus management, and anticonvulsant therapy.
- Headache Disorders: Migraine, tension-type headache, cluster headache, and trigeminal neuralgia.
- Movement Disorders: Parkinson’s disease, essential tremor, dystonia, and Huntington’s disease.
- Neurocognitive Disorders/Dementia: Alzheimer’s disease, vascular dementia, frontotemporal dementia, and delirium.
- Demyelinating Disorders: Multiple sclerosis (MS), Acute Disseminated Encephalomyelitis (ADEM), and Neuromyelitis Optica (NMOSD).
- Neuromuscular Disorders: Amyotrophic Lateral Sclerosis (ALS), peripheral neuropathy, myasthenia gravis, and muscular dystrophy.
- CNS Infections: Meningitis (bacterial, viral, fungal, TB), encephalitis, and brain abscess.
- Neuro-oncology: Primary brain tumors (gliomas, meningiomas) and brain metastases.
3. Specialized Topics and Emergencies
- Neurological Emergencies: Status epilepticus, acute stroke, intracranial hypertension, spinal cord compression, and GBS (Guillain-Barré syndrome).
- Neurocritical Care: Management of coma, brain death determination, and neurotrauma.
- Pediatric Neurology: Cerebral palsy, developmental delays, autism spectrum disorder, and childhood epilepsy.
- Neurogenetics: Familial dementias, Huntington’s disease, and hereditary neuropathies.
- Sleep Medicine: Narcolepsy, REM behavior disorder, and sleep apnea.
- Neuroimmunology: Autoimmune encephalitis and paraneoplastic syndromes.
4. Key Subspecialties
- Vascular Neurology (Stroke)
- Clinical Neurophysiology (EEG/EMG)
- Neuromuscular Medicine
- Child Neurology
- Neuro-oncology
- Neurocritical Care
- Behavioral Neurology
The core of a neurology clerkship or exam typically focuses heavily on 60-65% nervous system disorders, with remaining emphasis on musculoskeletal system interactions, behavioral health, and emergency assessment.
Gastrology for Physiotherapy and Nutrition Course
Gastroenterology (often referred to as gastrology in specific contexts) focuses on the diagnosis, treatment, and prevention of diseases related to the entire gastrointestinal (GI) tract—from the esophagus to the anus—as well as the liver, pancreas, gallbladder, and biliary tree.
Here are the main topics and core subjects in gastroenterology, categorized by system:
1. Upper Gastrointestinal (GI) Disorders
- Gastroesophageal Reflux Disease (GERD) & Barrett’s Esophagus: Chronic heartburn, acid suppression, and surveillance for cancer.
- Peptic Ulcer Disease (PUD): Ulcers caused by H. pylori or NSAIDs.
- Dysphagia & Gastroparesis: Swallowing disorders and delayed stomach emptying.
- Esophagitis: Inflammation of the esophagus, including eosinophilic esophagitis.
2. Lower Gastrointestinal (GI) Disorders
- Inflammatory Bowel Disease (IBD): Crohn’s disease and Ulcerative Colitis.
- Irritable Bowel Syndrome (IBS): Functional bowel disorder involving pain, constipation, or diarrhea.
- Colorectal Cancer & Polyps: Screening, detection, and removal.
- Diverticular Disease: Diverticulosis and acute diverticulitis.
- Malabsorption Syndromes: Celiac disease, lactose intolerance, and nutrient malabsorption.
- Infectious Gastroenteritis: C. difficile and other causes of diarrhea.
3. Hepatology (Liver Disease)
- Viral Hepatitis: Hepatitis B and Hepatitis C diagnosis and management.
- Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD/NAFLD): Fatty liver disease and its progressive forms (NASH).
- Cirrhosis & Portal Hypertension: Management of advanced liver fibrosis, ascites, and varices.
- Alcohol-Induced Liver Disease: Management and best practices.
4. Pancreatic and Biliary Diseases
- Pancreatitis: Acute and chronic pancreatic inflammation.
- Gallbladder Diseases: Gallstones (cholelithiasis) and cholecystitis.
- Cholestatic Syndromes: Primary biliary cholangitis (PBC).
- Pancreatic Cancer & Biliary Neoplasms: Tumors of the pancreas and bile ducts.
5. Specialized Procedures & Techniques
- Endoscopy: Upper endoscopy (EGD) and Lower endoscopy (Colonoscopy).
- Therapeutic Endoscopy: Polypectomy, Endoscopic Mucosal Resection (EMR), and stent insertion.
- Advanced Imaging: Endoscopic Ultrasound (EUS) and Endoscopic Retrograde Cholangiopancreatography (ERCP).
- Capsule Endoscopy: Imaging of the small intestine.
6. Functional and Emerging Topics
- Gut Microbiome: Role of flora in health and disease.
- Motility Disorders: Disorders of muscle movement in the gut, such as motility of the small intestine and colon.
- Nutrition: Enteral and parenteral nutrition support for GI patients.
- Medico-legal Issues: Ethics in GI care and endoscopy.
Electrotherapy for Physiotherapy and Nutrition Course
Electrotherapy is a core subject in physiotherapy that involves the therapeutic use of electrical currents, sound waves, or electromagnetic radiation to manage pain, reduce swelling, and stimulate muscle activity. It acts as an adjunct to manual therapy and exercise, requiring understanding of physics, physiology, and clinical application.
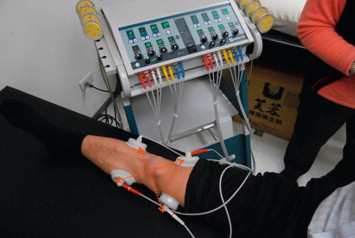
Here are the main topics and key components of an Electrotherapy curriculum:
1. Basic Principles of Electricity and Equipment
- Fundamental Physics: Understanding electrical currents, voltage, resistance (impedance), capacitance, and Ohm’s Law.
- Electrical Safety: Precautions regarding AC/DC current, earthing techniques, and preventing electrical/chemical burns.
- Electrophysiology: Principles of nerve and muscle excitation, action potentials, resting membrane potential, and strength-duration curves.
- Components & Waveforms: Types of currents (Direct, Alternating, Pulsed), waveforms, and frequency modulation.
- Electrodes: Types, sizes, coupling mediums, and placement techniques (bipolar, quadripolar).
2. Low-Frequency Currents (0-1000 Hz)
- TENS (Transcutaneous Electrical Nerve Stimulation): Used for pain modulation (Gate Control Theory, endorphin release).
- EMS (Electrical Muscle Stimulation): Used for strengthening weakened or denervated muscles.
- FES (Functional Electrical Stimulation): Used to re-educate functional movements.
- Iontophoresis: Using direct current to deliver ionized medication into tissues.
- Diadynamic Currents: Used for pain relief and stimulating nerve/muscle activity.
3. Medium-Frequency Currents (1-100 kHz)
- IFT (Interferential Therapy): Crossing medium-frequency currents to produce low-frequency effects deep in tissues, used for pain, edema, and blood flow.
- Russian Current/BMAC: Burst-modulated alternating current used for muscle strengthening.
4. High-Frequency Currents and Deep Heat
- SWD (Shortwave Diathermy): Using electromagnetic energy to produce deep heating, increasing metabolic activity and blood flow.
- MWD (Microwave Diathermy): Localized deep tissue heating.
- TECAR Therapy: Capacitive and resistive energy transfer for tissue repair.
5. Ultrasound Therapy and Mechanical Energy
- Therapeutic Ultrasound: Using high-frequency sound waves for thermal (deep heat) and non-thermal (cavitation, acoustic streaming) effects to aid soft tissue healing.
- Phonophoresis: Using ultrasound to drive medication through the skin.
- Shockwave Therapy (ESWT): Using acoustic waves to treat musculoskeletal conditions like tendonitis.
6. Electrodiagnosis
- Nerve Conduction Studies: Assessing motor and sensory nerve conduction velocity.
- Electromyography (EMG): Studying electrical activity of muscles to detect abnormalities.
- Strength-Duration (SD) Curve: Diagnostic plotting to determine the status of muscle innervation.
7. Other Electromagnetic and Light Agents
- LASER (Low-Level Laser Therapy): Photochemical effects for pain relief and tissue repair.
- UVR (Ultraviolet Radiation): Therapeutic applications for skin conditions and wound healing.
- IRR (Infrared Radiation): Superficial heat therapy.
8. Clinical Application and Safety
- Indications and Contraindications: Absolute and relative contraindications (e.g., pacemakers, pregnancy, malignancy, loss of sensation).
- Dosage Parameters: Setting intensity, frequency, pulse width, and treatment duration based on the condition (acute vs. chronic).
- Case Studies: Clinical decision-making in selecting appropriate modalities.
9. Superficial Heating and Cooling Modalities
- Cryotherapy: Using cold to reduce swelling, pain, and spasticity.
- Wax Therapy (Paraffin Wax Bath): Localized heat treatment.
- Hydrocollator Packs: Moist heat application.
- Contrast Bath: Alternating hot and cold to improve circulation.
10. Biofeedback
- EMG Biofeedback: Providing visual/audio information on muscle activity to enhance voluntary control.
Massage Therapy for Physiotherapy and Nutrition Course
A comprehensive massage therapy curriculum is structured around both theoretical knowledge and hands-on, practical skills. The core subjects focus on understanding the human body to ensure safe, effective, and ethical treatment.

Here are the main topics and subject areas in massage therapy, organized by category:
1. Foundational Sciences (The Anatomy & Physiology Core)
- Anatomy: Study of muscles, bones, joints, and connective tissues (fascia), with a focus on musculoskeletal structures, origin, insertion, and action of muscles.
- Physiology: Understanding how body systems (cardiovascular, lymphatic, nervous, endocrine) function and react to touch, including stress reduction and increased circulation.
- Pathology: Identification of common injuries (strains, sprains), illnesses, and, critically, contraindications (when massage should be avoided).
- Kinesiology: The study of human motion and biomechanics, essential for evaluating movement patterns and posture.
2. Massage Techniques & Modalities
- Swedish Massage: The foundation of Western massage, using long, flowing strokes (effleurage), kneading (petrissage), friction, vibration, and tapping (tapotement).
- Deep Tissue Massage: Techniques focusing on deeper layers of muscle tissue and fascia to relieve chronic tension.
- Sports Massage: Techniques designed for athletes to enhance performance, increase flexibility, and prevent or treat injuries.
- Specialized Modalities:
- Trigger Point Therapy: Addressing specific, tight “knots” causing referred pain.
- Myofascial Release: Gentle, sustained pressure on connective tissues.
- Hydrotherapy: The therapeutic use of heat (hot stone) and ice to reduce pain.
- Prenatal/Infant Massage: Specialized, safe techniques for expectant mothers.
- Chair Massage: Short, seated sessions often used in corporate settings.
3. Professionalism, Ethics & Safety
- Ethics & Boundaries: Maintaining client confidentiality, professional behavior, and establishing safe, respectful boundaries (including proper draping).
- Safety & Sanitation: Health, hygiene, and cleaning protocols to prevent the spread of illness.
- Client Assessment & Intake: Conducting interviews, observing posture, and creating treatment plans tailored to specific client needs.
- SOAP Charting: Documenting client sessions (Subjective, Objective, Assessment, Plan) for records and continuity of care.
4. Business Practices & Self-Care
- Business Management: Marketing, client retention, scheduling, and bookkeeping.
- Career Development: Resume building, legal requirements, insurance, and working in spas, clinics, or private practice.
- Self-Care for Therapists: Techniques for body mechanics to prevent injury and maintain longevity in the profession.
Exercise Therapy-1 for Physiotherapy and Nutrition Course
Exercise Therapy-1 (often called Fundamentals of Exercise Therapy or Basics of Therapeutic Exercise) is a core subject in physiotherapy, focusing on the techniques of restoring physical function, increasing range of motion, and improving muscle strength. It covers the foundational concepts, principles, and applications of movement as a treatment.
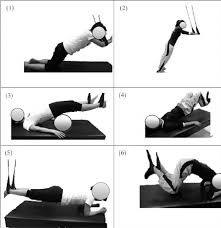
Here are the main topics generally covered in Exercise Therapy-1:
1. Foundations of Therapeutic Exercise
- Definition & Aims: Purpose of therapeutic exercise (e.g., pain relief, restoration of function, improving muscle power, preventing contractures).
- Components of Physical Fitness: Strength, endurance, flexibility, balance, and coordination.
- Models of Disability: Understanding the ICF (International Classification of Functioning, Disability, and Health) model—impairment, activity limitation, and participation restriction.
2. Biomechanics & Exercise Principles
- Positions: Fundamental starting positions (standing, sitting, kneeling, lying, hanging) and their derived positions.
- Joint Movement & Mechanics: Anatomical planes, axes of movement, levers, pulleys, and springs.
- Muscle Work: Classification of movements (active, passive, assisted, free) and muscle actions (concentric, eccentric, isometric).
3. Joint Mobility & Stretching Techniques
- Passive Movements: Techniques for relaxed passive movement, passive stretching, and CPM (Continuous Passive Motion).
- Stretching: Principles, types (static, dynamic, PNF), and indications for stretching to increase joint range.
- Joint Mobilization: Basics of assessment and mobilization techniques for upper/lower limbs.
- Goniometry: Measurement of joint range of motion (ROM) and identification of end-feels.
4. Muscle Performance & Strengthening
- Resistance Exercise: Principles of Progressive Resisted Exercise (PRE), including Oxford and Delorme methods.
- Types of Resistance: Manual, mechanical, isometric, and isokinetic training.
- Assessment: Manual Muscle Testing (MMT) grades (0 to 5).
5. Balance, Coordination & Posture
- Balance Training: Static and dynamic balance retraining, including wobbling boards and core stability exercises.
- Coordination Exercises: Frenkel’s exercises, non-equilibrium tests.
- Posture & Re-education: Principles of posture correction, postural awareness.
6. Functional & Special Modalities
- Suspension Therapy: Types of suspension, pulleys, and their application to increase range or strength.
- Gait Training: Normal gait cycle, walking aids (crutches, canes, frames), and gait training principles.
- Breathing Exercises: Diaphragmatic, segmental, and pursed-lip breathing.
- Relaxation Techniques: General and local techniques (e.g., Jacobson’s, Mitchell’s).
- Therapeutic Massage: Principles, types, and application of massage for relaxation and therapeutic effect.
- Hydrotherapy: Principles of aquatic exercise.
7. Safety & Evaluation
Patient Assessment: Assessment of vital signs (blood pressure, pulse, respiration), sensation, and anthropometric measurements (girth, length).
Contraindications & Precautions: Identifying when not to use specific exercises.
Electrotherapy-2 for Physiotherapy and Nutrition Course
Electrotherapy-2 (often titled “Physical Agents & Electrotherapy II” or “Advanced Electrotherapy”) generally focuses on medium-to-high frequency currents, deep heating modalities, light therapies, and advanced electro-diagnosis. It follows Electrotherapy-1, moving beyond basic low-frequency currents (TENS/Faradic) into more complex applications.

Here are the main topics covered in Electrotherapy-2:
1. Medium Frequency Currents
- Interferential Therapy (IFT): Principles of interference, amplitude-modulated frequency (AMF), beat frequency, carrier frequency (typically 4000 Hz), quadripolar vs. bipolar application, and scanning/sweep techniques.
- Russian Currents & Aussie Currents: Principles, application for strengthening, and muscle stimulation techniques.
- Diadynamic Currents: Characteristics, types (MF, DF, CP, LP), and therapeutic applications.
2. High-Frequency Currents (Deep Heat Therapy)
- Shortwave Diathermy (SWD): Principles of capacitance and inductance, techniques of application (capacitor field/electrodes, cable method), pulsed shortwave therapy (PSWT), contraindications, and dangers.
- Microwave Diathermy (MWD): Production, applicators, physiological effects, and dangers.
- Therapeutic Ultrasound (US): Principles of production (reverse piezoelectric effect), thermal and non-thermal effects, coupling media (gels, water bath), phonophoresis, and dosage.
3. Light and Radiation Therapy (Actinotherapy)
- Laser Therapy (Low-Level Laser Therapy – LLLT): Types of laser (HeNe, Ruby), properties (coherence, monochromaticity), physiological effects, techniques of application, and safety precautions.
- Ultra Violet Radiation (UVR): Types (UVA, UVB, UVC), ultraviolet generators (mercury vapor lamps, fluorescent tubes), minimal erythemal dose (MED), PUVA, and UVR for skin conditions.
- Infrared Radiation (IRR): Luminous and non-luminous generators, properties, and physiological effects.
4. Advanced Electro-diagnosis & Stimulation
- Strength-Duration (SD) Curve: Factors affecting accuracy, clinical significance in peripheral nerve injury, and diagnosis of nerve lesions.
- Electromyography (EMG): Basics of motor unit potentials, recording electrodes, and clinical applications.
- Nerve Conduction Velocity (NCV): H-reflex and F-wave studies.
- Electrical Stimulation of Denervated Muscle: Long-duration impulses.
5. Other Modalities & Techniques
- Cryotherapy & Cryokinetics: Physiological effects, ice massage, ice packs, and ice baths.
- Hydrotherapy: Whirlpool bath, contrast bath, Hubbard tank, and wax therapy (paraffin wax bath).
- Mechanical Modalities: Mechanical traction (cervical/lumbar), compression therapy (intermittent compression pumps).
- Biofeedback: Principles and clinical applications.
6. Clinical Application & Safety
- Pain Mechanisms: Gate Control Theory, Endogenous Opiate Release.
- Wound Healing: Use of microcurrents, high-voltage pulsed galvanic current (HVPGC), and electrical stimulation for tissue repair.
- Contraindications & Safety: Dangers of high-frequency currents, contraindications for metallic implants, pacemakers, and pregnancy.
Orthopedics for for Physiotherapy and Nutrition Course
Orthopedics involves the diagnosis, treatment, and rehabilitation of musculoskeletal disorders, focusing on bones, joints, ligaments, tendons, and muscles. Key topics include fracture management, joint replacements (arthroplasty), sports medicine, spinal disorders, pediatric deformities, and bone tumors. Key areas to master are Trauma, Infections, and Metabolic Bone Diseases.
Core Orthopedic Subject Areas
- Trauma and Fracture Management: General principles, management of open fractures, compartment syndrome, fat embolism, and specific fractures (e.g., hip, femur, supracondylar humerus, Colles, scaphoid).
- Joints and Arthritis: Osteoarthritis, rheumatoid arthritis, gout, and joint replacements (arthroplasty) for knee, hip, and shoulder.
- Pediatric Orthopedics: Congenital disorders (e.g., Clubfoot/CTEV, Developmental Dysplasia of the Hip/DDH), growth plate injuries (Salter-Harris classification), and Rickets.
- Spine Disorders: Intervertebral disc prolapse, spinal injuries (cervical spine), Pott’s spine (tuberculosis), and scoliosis.
- Infections and Tumors: Acute and chronic osteomyelitis, pyogenic arthritis, and bone tumors (benign, malignant, osteoclastoma).
- Metabolic Bone Diseases: Osteoporosis, osteomalacia, Paget’s disease, and hyperparathyroidism.
- Sports Medicine and Soft Tissue: Ligament injuries (ACL/Meniscal injuries), rotator cuff tears, and tendonitis.
- Hand, Foot, and Nerve Injuries: Carpal tunnel syndrome, nerve injuries (radial, ulnar, median), foot deformities, and Dupuytren’s contracture.
High-Yield Topics for Exams
- Management of Traumatic Paraplegia
- Bone Tumors (diagnosis and classification)
- Compound (Open) Fracture Management
- Congenital Dislocation of Hip (CDH/DDH)
- Internal Fixation Techniques
Key Principles
- 4 A’s of Orthopedic Surgery: Anatomy, Alignment, Asepsis, and Anesthesia.
- Rehabilitation: Post-operative care, physiotherapy, and prosthetic devices.
Vitamin Deficiency Diseases for Physiotherapy and Nutrition Course
Vitamin deficiency diseases are medical conditions caused by an inadequate intake or poor absorption of essential vitamins over a prolonged period. They are categorized based on whether the vitamin is water-soluble (needs daily replenishment) or fat-soluble (stored in the body).
Here is a structured overview of the main topics in vitamin deficiency diseases:
1. Key Vitamin Deficiency Diseases & Related Deficiencies
- Vitamin A (Retinol) Deficiency: Causes Night Blindness, xerophthalmia (dry eyes), Bitot spots, and increased infection susceptibility.
- Vitamin B1 (Thiamine) Deficiency: Causes Beriberi (cardiovascular and nerve damage) and Wernicke-Korsakoff syndrome.
- Vitamin B2 (Riboflavin) Deficiency: Causes Ariboflavinosis (retarded growth, skin problems, swollen throat, mouth sores).
- Vitamin B3 (Niacin) Deficiency: Causes Pellagra (characterized by the “4 Ds”: dermatitis, diarrhea, dementia, and death).
- Vitamin B6 Deficiency: Leads to anemia, peripheral neuropathy, and skin disorders.
- Vitamin B9 (Folate) Deficiency: Causes Megaloblastic Anemia and is linked to neural tube defects in newborns.
- Vitamin B12 (Cyanocobalamin) Deficiency: Causes Pernicious Anemia, neurological issues, and cognitive impairment.
- Vitamin C (Ascorbic Acid) Deficiency: Causes Scurvy (bleeding gums, petechiae, impaired wound healing).
- Vitamin D (Calciferol) Deficiency: Causes Rickets in children (bone deformities) and Osteomalacia in adults (soft bones).
- Vitamin E Deficiency: Causes neurological issues, ataxia, and hemolytic anemia.
- Vitamin K Deficiency: Causes Coagulation Disorders (excessive bleeding).
2. Major Causes of Vitamin Deficiencies
- Poor Diet/Nutritional Inadequacy: Consuming processed foods, lack of variety, or poverty.
- Malabsorption Syndromes: Conditions such as Crohn’s disease, Celiac disease, or chronic alcohol use disorder hinder nutrient absorption.
- Increased Requirements: Pregnancy, lactation, or rapid growth in children can increase the need for specific vitamins.
- Lifestyle & Environmental Factors: Lack of sunlight exposure (Vitamin D) or strict vegetarian/vegan diets (Vitamin B12).
3. Common Symptoms Across Deficiencies
- Fatigue and Weakness: Common across most deficiencies.
- Skin, Hair, and Nail Changes: Rashes, dermatitis, alopecia, brittle nails.
- Neurological Issues: Numbness, tingling (paresthesia), cognitive impairment.
- Immune System Dysfunction: Slow wound healing and increased susceptibility to infections.
4. Diagnosis and Treatment
- Diagnosis: Primarily through blood tests, clinical history, and symptom analysis.
- Treatment: Dietary modifications (consuming nutrient-dense foods) and supplementation (oral or injections).
5. Risk Factors & Vulnerable Populations
- Elderly: Due to reduced absorption.
- Pregnant and Lactating Women: Due to higher nutritional needs.
- Individuals with Chronic Illnesses: Digestive disorders, kidney diseases.
6. Prevention Strategies
- Balanced Nutrition: Consuming a diverse diet.
- Food Fortification: Public health programs that add vitamins to common foods (e.g., Vitamin D in milk).
- Supplementation Programs: Targeted initiatives for high-risk groups.
Mineral Deficiency Diseases for Physiotherapy and Nutrition Course
Mineral deficiency diseases result from an inadequate intake or poor absorption of essential inorganic nutrients. These deficiencies can cause severe health complications, developmental delays in children, and chronic diseases. The most significant, widespread, and commonly studied mineral deficiencies are iron, iodine, calcium, zinc, and magnesium.
Here is a structured overview of the main topics in mineral deficiency diseases:
1. Key Mineral Deficiencies & Associated Diseases
- Iron Deficiency (Anaemia): The most common nutrient deficiency worldwide. It leads to iron-deficiency anemia, characterized by fatigue, weakness, pale skin, brittleness of nails, and impaired immune function.
- Iodine Deficiency (Goitre/Hypothyroidism): Causes goitre (enlarged thyroid gland), hypothyroidism, and, if severe during pregnancy, irreversible mental retardation and cretinism in offspring.
- Calcium Deficiency (Hypocalcemia/Osteoporosis): Causes brittle bones, weak teeth, osteopenia, and osteoporosis. It also causes muscle cramps, palpitations, and in severe cases, tetany.
- Zinc Deficiency: Leads to impaired immune function, delayed wound healing, loss of appetite, hair loss, and skin lesions. It is a major cause of stunted growth in children.
- Magnesium Deficiency (Hypomagnesemia): Causes muscle cramps, spasms, tremors, fatigue, and is linked to metabolic syndrome, diabetes, and hypertension.
- Potassium Deficiency (Hypokalemia): Causes muscle weakness, constipation, and irregular heartbeats.
- Selenium Deficiency: Implicated in Keshan disease (cardiomyopathy) and Kashin-Bek disease (deforming arthritis).
- Fluoride Deficiency: Results in increased susceptibility to dental caries (tooth decay).
2. Common Causes of Mineral Deficiencies
- Poor Diet/Inadequate Intake: Diets low in nutrient-dense foods (e.g., lack of fruits, vegetables, or animal products).
- Malabsorption Disorders: Conditions like celiac disease, Crohn’s disease, inflammatory bowel disease (IBD), or bariatric surgery.
- Increased Requirements: Pregnancy, lactation, and rapid growth in childhood.
- Medications: Prolonged use of diuretics or antacids.
3. General Symptoms of Mineral Deficiencies
- Fatigue and weakness
- Skin, hair, and nail changes (e.g., hair loss, brittle nails, rashes)
- Muscle effects (e.g., cramps, spasms, weakness)
- Neurological symptoms (e.g., numbness, tingling, cognitive impairment)
- Impaired immune system
4. Diagnosis and Treatment
- Diagnosis: Blood tests (serum ferritin for iron, TSH for iodine), urine tests, and dietary history assessment.
- Treatment: Dietary modification (fortified foods), supplementation, and treatment of underlying malabsorption disorders.
- Prevention: Public health initiatives like food fortification (e.g., iodized salt, iron-fortified flour) and nutritional education.
5. At-Risk Populations
- Pregnant Women: High risk of iron and iodine deficiencies, impacting fetal development.
- Children: Vulnerable to stunted growth and cognitive impairment.
- Elderly: Often at risk due to reduced food intake or absorption issues.
- Vegetarians/Vegans: May lack specific minerals like iron and zinc.
6. Consequences of Untreated Deficiencies
If left untreated, mineral deficiencies can lead to long-term health problems such as:
- Irreversible cognitive decline (especially iodine)
- Permanent bone loss (osteoporosis)
- Chronic cardiovascular conditions
- Severe developmental delays in children
Hyper Vitaminosis & Treatment for Physiotherapy and Nutrition Course
Hypervitaminosis A, or vitamin A toxicity, is a condition caused by the excessive accumulation of preformed vitamin A (retinol/retinyl esters) in the body, primarily stored in the liver. Treatment focuses on removing the source of excess and providing supportive care to manage symptoms.
Primary Treatment Approaches
- Immediate Discontinuation: The most critical step is stopping all vitamin A supplements, fortified foods, and medication sources (e.g., retinoids, fish liver oils).
- Supportive Care: Because there is no specific antidote for vitamin A toxicity, care is generally symptomatic.
- Hospitalization: In severe or acute cases (especially in children), hospitalization may be required for stabilization.
- Liver Transplantation: In extreme cases resulting in liver failure or severe cirrhosis, a liver transplant may be necessary.
Management of Specific Symptoms/Complications
- Increased Intracranial Pressure (Pseudotumor Cerebri): Treated with head elevation and potentially acetazolamide.
- Hypercalcemia: Managed through hydration, reduced calcium intake, and potentially bisphosphonates.
- Skin and Hair Changes: Symptoms like dry skin, cheilitis (cracked lips), and alopecia typically resolve upon stopping the intake of excess vitamin A.
- Hepatic Damage: Monitored via liver function tests.
- Nutritional Support: Vitamin E has been suggested to have some therapeutic benefit in treating vitamin A toxicity.
Diagnosis and Monitoring
- Laboratory Tests: Serum vitamin A levels, retinyl ester levels, and liver function tests are used to confirm toxicity.
- Monitoring: Follow-up checks of vitamin A levels are recommended after 3 months, with annual checks for those with a history of toxicity.
Prognosis and Recovery
- Recovery Timeline: Symptoms generally resolve within a few weeks to months after discontinuing the vitamin A source.
- Irreversible Damage: Chronic, severe toxicity can lead to permanent damage, such as cirrhosis or liver fibrosis.
- Pregnancy Risks: High intake during pregnancy can cause birth defects, which are irreversible.
Prevention
- Safe Intake Limits: Avoid exceeding the Tolerable Upper Intake Level (UL) of 3000 RAE (10,000 IU) per day for adults.
- Dietary Awareness: Be cautious with foods very high in Vitamin A, such as liver.
- Supplement Review: Check all supplements and medications for high doses of preformed Vitamin A.
Carbohydrate Metabolic Disease for Physiotherapy and Nutrition Course
Carbohydrate metabolic diseases are a group of metabolic disorders, usually inherited (inborn errors of metabolism), that disrupt the body’s ability to properly break down, store, or utilize carbohydrates for energy. These disorders often stem from enzyme deficiencies that cause harmful sugars (like galactose or fructose) to build up in the body, leading to potential liver dysfunction, kidney disease, or developmental delays.
Here are the main topics and key diseases within the subject of Carbohydrate Metabolic Disease:
1. Core Inborn Errors of Carbohydrate Metabolism
These are genetic disorders involving specific metabolic pathway defects.
- Galactosemia: A disorder where the body cannot metabolize galactose (a sugar found in lactose). It is caused by a deficiency in enzymes like galactose-1-phosphate uridyltransferase.
- Glycogen Storage Diseases (GSDs): A group of disorders (e.g., Von Gierke’s disease, Pompe disease) where the body cannot properly break down or store glycogen in the liver and muscles.
- Hereditary Fructose Intolerance (HFI): A condition caused by a lack of the enzyme aldolase B, which is essential for breaking down fructose.
- Pyruvate Metabolism Disorders: Metabolic defects affecting the conversion of pyruvate, which can lead to lactic acidosis.
- Mucopolysaccharidoses (MPS): Genetic disorders involving the inability to break down complex sugars (e.g., Hunter or Hurler syndromes).
2. Common Acquired Carbohydrate Disorders
While some diseases are inherited, others are acquired due to lifestyle or metabolic dysfunction.
- Diabetes Mellitus (Types 1, 2, & Gestational): A chronic condition characterized by high blood glucose (hyperglycemia) resulting from issues with insulin production or sensitivity.
- Lactose Intolerance: A very common, often age-related condition due to insufficient lactase enzyme production.
- Hypoglycemia: Low blood sugar, which can be caused by various metabolic issues, including hyperinsulinism.
- Fructose Malabsorption: A condition where the small intestine cannot properly absorb fructose.
3. Key Metabolic Pathways & Processes
Understanding the normal processes is essential to identifying where the metabolic breakdown occurs.
- Glycolysis: The breakdown of glucose to produce energy.
- Glycogenesis/Glycogenolysis: The synthesis and breakdown of glycogen, respectively.
- Gluconeogenesis: The formation of glucose from non-carbohydrate precursors (like lactate or amino acids).
- Pentose Phosphate Pathway: An alternative pathway for glucose oxidation.
4. Diagnosis and Management
- Newborn Screening: Blood tests to identify inborn errors early to prevent severe, irreversible damage.
- Dietary Management: The primary treatment for many disorders, such as eliminating lactose (galactosemia) or fructose, sucrose, and sorbitol (HFI).
- Genetic Testing: Used to identify inherited gene mutations.
- Enzyme Assays/Biopsies: Used to determine specific enzymatic activity levels in organs like the liver.
5. Symptoms and Complications
- Metabolic Crisis: Severe hypoglycemia, vomiting, lethargy, and jaundice in neonates.
- Hepatomegaly: Enlarged liver, common in GSDs and HFI.
- Myopathy: Muscle weakness or pain, often seen in GSDs (e.g., Pompe disease).
- Cataracts: A common symptom of galactosemia.
Practical Classes for Physiotherapy and Nutrition Course
Auscultation, Heart Beat, Heart Rate, Heart Sound, Pulse, Blood Pressure, Respiratory Rate, Inhaler, Rota Haler, Nebulizer, Blood Oxygen, Cyanosis, Blood Glucose (Diabetes), Body Temperature, Dehydration Test, Edema Test, Jaundice test, Anemia test, IM Injection, IV Injection, SC Injection, ID Injection, Saline Infusion, Cleaning, Dressing, Bandaging, Oxygen by Pulse Oximeter, TENS, IRR, Short Wave Therapy, etc.
Practical Class on Heartbeat
A heartbeat is the rhythmic contraction and relaxation of the heart, driven by electrical signals, pumping blood through the body; it involves phases like diastole (relaxation/filling) and systole (contraction/pumping) and is measured as beats per minute (BPM), with 60-100 BPM being a normal resting range for adults, though it varies with activity. The electrical impulse originates at the sinoatrial (SA) node, travels through the atria, and then to the ventricles, causing them to contract and pump oxygenated and deoxygenated blood.
How it works (The Cardiac Cycle)
- Diastole (Relaxation): The heart’s chambers relax, and blood flows from the body into the right atrium and from the lungs into the left atrium, then into the ventricles.
- Atrial Systole: The atria contract, pushing remaining blood into the ventricles.
- Ventricular Systole: The ventricles contract forcefully, pushing blood out: the right side sends it to the lungs, and the left side pumps it to the rest of the body.
- Cycle Repeats: The heart then re-enters diastole, refilling with blood.
Key Terms
- SA Node: The heart’s natural pacemaker, initiating the electrical signal.
- Pulse: The palpable wave of blood flow from the heart’s beat.
- Heart Rate: The number of beats per minute (BPM).
- Tachycardia: A heart rate over 100 BPM at rest.
- Bradycardia: A slow heart rate (not mentioned in snippets, but implied opposite of tachycardia).
What affects it
- Factors Such as Stress, caffeine, nicotine, exercise, and hormones can increase heart rate.
- Normal Range: 60-100 BPM at rest for most adults, though athletes often have lower rates.
Practical Class on Heart Rate
Heart rate is the number of times your heart beats per minute (bpm), with a normal resting rate for adults generally being 60-100 bpm, though it varies with age, fitness, stress, and medications, with athletes often having lower rates. It’s a key health indicator, reflecting heart function; a consistently high rate (tachycardia, >100 bpm at rest) or low rate (bradycardia, <60 bpm at rest, unless fit) can signal issues. You can check it by feeling your pulse at the wrist or with devices, ideally after resting.
Normal Ranges & Factors
- Adults: 60-100 bpm resting.
- Athletes: Can be as low as 40 bpm or less.
- Children: Have higher rates, e.g., 80-120 bpm for ages 3-5.
- Factors Affecting It: Fitness, emotions, caffeine, alcohol, medications, illness, pregnancy, and sleep quality.
How to Check Your Heart Rate
- Rest: Sit quietly for 5-10 minutes.
- Locate Pulse: Place index and middle fingers on the thumb side of your wrist.
- Count: Count beats for 15 seconds and multiply by 4, or count for a full minute.
- Devices: Smartwatches and fitness trackers offer easy monitoring.
Practical Class on Tachycardia
Tachycardia is a heart rhythm disorder where the heart beats too fast, typically over 100 beats per minute (bpm) at rest in adults, signaling an electrical problem or normal response to stress, exercise, or underlying conditions like fever, anemia, anxiety, or thyroid issues, causing symptoms like palpitations, dizziness, and shortness of breath, requiring medical evaluation to determine if it’s benign (sinus tachycardia) or a serious arrhythmia needing treatment.
Types of Tachycardia
- Sinus Tachycardia: A normal response to stress, fever, or exercise, where the sinus node fires too quickly.
- Supraventricular Tachycardia (SVT): Abnormal signals start above the ventricles, causing sudden, rapid heartbeats, often felt as palpitations.
- Ventricular Tachycardia (VT): A dangerous rhythm originating in the heart’s lower chambers, potentially life-threatening.
- Atrial Fibrillation (AFib) & Flutter: Irregular, rapid heartbeats in the upper chambers (atria).
Common Symptoms
Racing heart or palpitations, Dizziness or lightheadedness, Shortness of breath, and Chest pain or discomfort.
Common Causes & Triggers
- Lifestyle: Caffeine, alcohol, stimulants, smoking, stress, lack of sleep.
- Medical Conditions: Fever, anemia, thyroid disease, dehydration, lung disease, sleep apnea, heart disease, and high blood pressure.
- Electrical Issues: Faulty heart wiring or triggers in the heart’s chambers.
Practical Class on Bradycardia
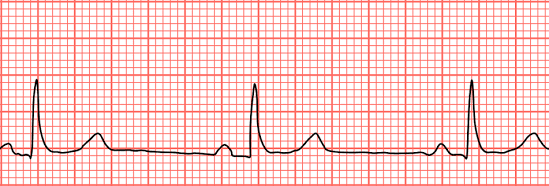

Bradycardia is a slower-than-normal heart rate, typically under 60 beats per minute (bpm) in adults at rest, caused by issues with the heart’s electrical system, certain medications, or underlying conditions like sleep apnea or thyroid problems, leading to symptoms like dizziness, fatigue, shortness of breath, and confusion, though highly fit individuals and athletes may have a normal slow rate. Treatment varies by cause, ranging from lifestyle changes to pacemakers, and involves diagnosing the underlying problem with tools like an EKG.
What it is
- A heart rate below 60 bpm, meaning the heart isn’t pumping enough oxygen-rich blood to the body.
- Can be normal for athletes or during sleep, but problematic if it causes symptoms.
Common types
- Sinus Bradycardia: Slowing of the heart’s natural pacemaker (sinus node).
- Heart Block: Electrical signals from the upper to lower heart chambers are blocked.
Causes
- Heart Issues: Heart disease, previous heart attacks, sick sinus syndrome.
- Medications: Beta-blockers, calcium channel blockers.
- Medical Conditions: Thyroid problems, electrolyte imbalances, sleep apnea, and inflammation.
- Lifestyle: Intense physical fitness (often normal), aging.
Symptoms (when problematic)
- Dizziness, lightheadedness, fainting.
- Fatigue, weakness.
- Shortness of breath, chest pain.
- Confusion or memory problems.
Diagnosis & Treatment
- Diagnosis: Physical exam, EKG, Holter monitor, sleep study, blood tests.
- Treatment: Addressing the cause (e.g., changing meds, treating sleep apnea) or using a pacemaker for severe cases.
Practical Class on IM Injection Pushing
The process of pushing an intramuscular (IM) injection involves a smooth, steady depression of the plunger after the needle is securely in the muscle, ensuring the medication goes in slowly to minimize discomfort, followed by quickly withdrawing the needle at the same angle and activating the safety device, then applying gentle pressure to the site with gauze. Key steps include site preparation (cleaning, Z-track method), swift 90-degree needle insertion, slow plunger push (counting to three), quick withdrawal, and immediate disposal in a sharps container.
Pre-Injection Steps (Preparation)
- Hand Hygiene & Supplies: Wash hands thoroughly and gather medication, syringe, alcohol swabs, gauze, and a sharps container.
- Site Selection & Prep: Locate the correct muscle (e.g., deltoid, ventrogluteal), clean with an alcohol swab, and let it dry.
- Z-Track Method (Optional but Recommended): Use your non-dominant hand to pull the skin and tissue to the side to prevent medication leakage into subcutaneous tissue.
- Syringe Prep: Remove the cap, ensure no large air bubbles, and tap to get a drop of medication at the tip.
The “Push” (Injection)
- Insertion: Hold the syringe like a dart and insert the needle quickly at a 90-degree angle into the muscle.
- Stabilize: Once in the muscle, use your non-dominant hand to steady the syringe.
- Depress Plunger: Slowly and steadily push the plunger all the way down, counting to three.
- Withdrawal: After the fluid is in, hold for a few seconds (around 10 for some meds), then pull the needle straight out at the same 90-degree angle.
Post-Injection Steps
- Safety: Immediately activate the needle’s safety shield and dispose of the entire syringe in the sharps container.
- Site Care: Apply gentle pressure with gauze or a cotton ball (no rubbing) and secure with a bandage if needed.
- Observe: Monitor the patient for any adverse reactions.
Process of IV Injection Pushing
The process of IV Injection Pushing (or Bolus) involves a trained healthcare professional manually injecting medication directly into an established IV line using a syringe, following strict steps: verify order, prepare patient, scrub the IV port (clave), flush with saline to check for patency, attach the medication syringe, push the drug at a specific rate (seconds to minutes) while monitoring, and then perform a post-flush to clear the line, ensuring patient safety and proper delivery.
Key Steps in IV Push Administration
- Preparation & Verification:
- Confirm the doctor’s order, patient details, medication rights (right drug, dose, time, route, patient, documentation, reason, response).
- Gather supplies: saline flush, medication syringe, alcohol wipes, and gloves.
- Perform hand hygiene and don gloves.
- Educate the patient about the medication and potential side effects.
- Priming & Flushing (SASH Method):
- Saline Flush: Scrub the injection port (clave) with an alcohol wipe for 15-30 seconds, let it air dry, then inject 3-5mL of saline to check for patency (blood return) and clear the line.
- Medication Administration:
- Attach Medication: Attach the pre-filled medication syringe (air expelled) to the scrubbed port and twist clockwise to secure.
- Slow Push: Slowly inject the medication at the prescribed rate (e.g., over 1 minute, 2 minutes). Use a timer for accuracy; break down the volume into smaller intervals for easier pacing (e.g., 0.5mL every 30 seconds for a 1mL/min push).
- Completion (SASH):
- Follow-up Flush: After the medication, flush with another 3-5mL of saline at the same rate as the medication push to ensure all the drug enters the bloodstream and clears the tubing, preventing incompatibility with other IV fluids.
- Secure the port with a new alcohol cap if required by facility policy.
Important Considerations
- Timing is Crucial: Pushing too fast can cause adverse effects or medication waste; too slow might delay treatment.
- Compatibility: Always check if the medication is compatible with the primary IV fluid running, if any.
- Patient Monitoring: Closely watch the patient for any adverse reactions during and after administration, especially respiratory changes, notes LevelUpRN.
Practicle class for TENS
This TENS (Transcutaneous Electrical Nerve Stimulation) practical guide is
designed for physiotherapy students and professionals, focusing on the clinical application of pain management. TENS is a non-invasive, drug-free method used to stimulate sensory nerves, activating the pain gate mechanism or endorphin release to alleviate acute and chronic pain.
1. Preparation and Setup
- Patient Assessment: Evaluate the pain site, type (acute/chronic), and rule out contraindications (e.g., pacemakers, epilepsy, epilepsy, or over carotid sinus).
- Skin Prep: Ensure the skin is clean, dry, and free of lesions or excessive hair (shaving may be required). Apply conductive gel if using carbon electrodes.
- Electrode Placement:
- Directly over pain: Place pads around the pain site.
- Over nerve pathway: Along the sensory nerve path.
- Dermatome/Spinal Level: Corresponding to the nerve root.
- Crossing Pattern (Quadripolar): Using 4 electrodes from 2 channels, cross them directly over the pain center for maximum coverage.
- Unit Check: Ensure the unit is off before placing pads, and check batteries.
2. TENS Modes and Parameters (The “Toolkit”)
Physiotherapists select parameters based on the pain type:
- Conventional TENS (High Frequency):
- Frequency: 90–130 Hz.
- Pulse Width: 50–100
𝜇s.
- Goal: Immediate relief, “tingling” sensation (sensory).
- Acupuncture-like TENS (Low Frequency):
- Frequency: 2–10 Hz.
- Pulse Width: 150–250
𝜇s.
- Goal: Longer-lasting relief (endorphin release).
- Burst Mode TENS:
- Setting: High frequency (100Hz) delivered in bursts (2–3 bursts/sec).
- Goal: Good for chronic pain; combines gate control and endorphin release.
3. Practical Application Steps
- Select Mode: Choose Conventional, Low, or Burst, based on patient comfort and pain type.
- Turn on Channel 1: Gradually increase intensity until the patient feels a “strong but comfortable” tingling sensation. Avoid producing muscle twitching if using conventional mode.
- Turn on Channel 2 (if needed): Repeat for the second pair of electrodes.
- Treatment Duration: Typically 30–60 minutes, up to several times a day.
- Remove Electrodes: Turn off the unit first, then gently peel off electrodes.
4. Safety Precautions
- Never place electrodes over: The anterior neck (carotid sinus), eyes, or directly over a pacemaker.
- Contraindicated for: Patients with epilepsy or cognitive impairment who cannot understand the instructions.
- Avoid in: Early pregnancy (trunk/abdomen).
5. Clinical Tips
- “Strong but comfortable” is the golden rule for intensity.
- If the patient becomes accustomed to the sensation, adjust the frequency or switch modes to maintain effectiveness.
- TENS is most effective when combined with therapeutic exercise and manual therapy.
 HRTD Medical Institute
HRTD Medical Institute





